Antimicrobial resistance
Antimicrobial resistance (AMR) is the resistance of a microorganism to an antimicrobial medicine to which it was previously sensitive. It develops when a microorganism mutates or acquires a resistance gene. Resistant organisms (including bacteria, viruses, fungi, protozoa and helminths) are able to withstand attack by antimicrobial medicines such as antibiotics, antivirals and antimalarials, so that standard treatments become ineffective and infections persist and may spread to other people.
About AMRTop story
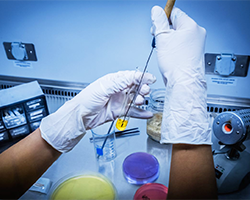 New WHO tools use behavioural insights to help curb the spread of antimicrobial resistance
New WHO tools use behavioural insights to help curb the spread of antimicrobial resistance
WHO has released 3 documents that aim to strengthen efforts to tackle antimicrobial resistance (AMR) through a behavioural insights approach: the TAP Quick Guide, the TAP Toolbox and the TAP Process poster. A fourth document – the TAP Manual – will be available by the end of the year.
Advocacy briefs

AMR affects health in different contexts and focusing on different sectors can contribute to managing AMR.
Download the suite of advocacy documentsMultimedia
Video - Antibiotics don’t work on viruses like influenza
Key resource
Central Asian and European Surveillance of Antimicrobial Resistance network (CAESAR)A joint initiative to survey, contain and prevent the emergence and spread of antibiotic resistance in the European Region.
Publications
 Central Asian and European Surveillance of Antimicrobial Resistance. Annual report 2019
More publications
Central Asian and European Surveillance of Antimicrobial Resistance. Annual report 2019
More publications
Data and statistics
33,000
The number of people who die every year in EU/EEA countries due to an infection with a resistant bacterial strain. Estimate for the whole WHO European Region is currently not available.